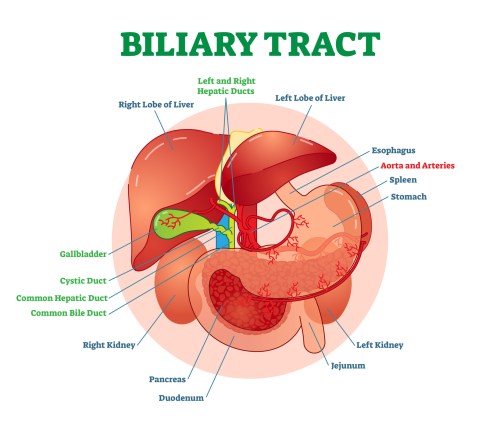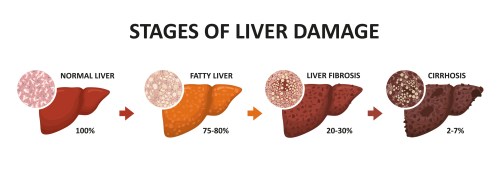
Stages of liver damage. Healthy, fatty, liver fibrosis, and finally cirrhosis
A recent article in Gastroenterology Clinics suggests this one:
•Prioritize intact starches such as brown rice, quinoa, and steel-cut oats, and limit or avoid refined starches such as white bread and white rice
•Replace some of the CHO [carbohydrate], especially refined CHO, in the diet with additional protein from a mixture of animal or vegetable sources, including chicken, fish, cheese, tofu, and pulses
•Include a variety of bioactive compounds in the diet by consuming fruits, vegetables, coffee, tea, nuts, seeds, and extra virgin olive oil
•Get most fat from unsaturated sources, such as olive oil (ideally extra virgin), rapeseed oil, sunflower oil, safflower oil, canola oil, or nuts and seeds
•Limit or avoid added sugars, whether sucrose, fructose, maltose, maltodextrin, or any syrups. If any of these words appear in the first 3–5 ingredients of any food item, it is best to avoid that item and choose a no-sugar version instead. Examples are yogurts and commercial cereals•In particular, avoid liquid sugar such as carbonated sugary drinks/sodas, lemonade, any juices, smoothies, and added sugar to tea and coffee
Source: Nutrition and Nonalcoholic Fatty Liver Disease – Gastroenterology Clinics
See the article for a typical daily menu. Looks like a Mediterranean diet to me.
Excessive fructose and saturated fatty acid consumption appear to be particularly harmful to the liver.
The authors also seem to endorse exercise: 150 t0 300 minutes per week of moderate- to vigorous intensity aerobics exercise, performed at least thrice weekly.
And all experts recommend loss of excess fat weight.
If you really want to get into the weeds, click the link above to read about how fat deposits in liver and muscle lead to metabolic inflexibility, resulting in insulin resistance and mitochondrial dysfunction, which alters lipid metabolism, releasing free fatty acids (some of which are lipotoxic), leading to lipotoxic molecules (like ceramides), causing inflammation and fibrosis.
Steve Parker, M.D.

Click the pic to purchase at Amazon.com. E-book versions also available at Smashwords. com.